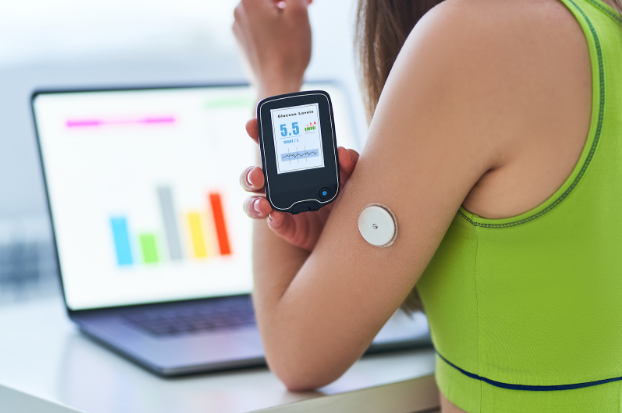
Nighttime CGM: Managing Nocturnal Blood Sugar with Wearables
|
|
Time to read 8 min
|
|
Time to read 8 min
Diabetes, being as common as it is, is one of the most frustrating diseases to deal with. Fortunately, there are several convenient ways to manage it.
One of the latest diabetes technology methods to battle some uncommon but serious complications of diabetes is using a nighttime CGM (continuous glucose monitoring) to measure blood glucose levels.
These wearable devices will allow you to reduce the instances of finger-prick blood glucose meter tests and give you a lot more assurance while resting at night.
Let's begin by understanding what they are and their importance.
Nighttime wearables, or continuous glucose monitors or CGMs, are sensors you place under your skin to constantly measure your blood sugar.
CGM devices aren't to be confused with insulin pumps, as their purpose in diabetes management is to measure the patient's blood glucose levels, not administer insulin.
When these sensors first came to be, they were somewhat bulky, which made it difficult to keep them on while sleeping.
However, with some upgrades, continuous glucose monitors are now small enough to be placed under skin patches or even implanted to monitor nocturnal blood sugar. Some examples of such devices are:
All of those devices are small enough to be worn whether you're awake or sleeping.
Nocturnal continuous glucose monitoring is crucial due to the possibility of hypoglycemia, a condition that occurs when the blood sugar drops below 4 mmol/L or 72 mg/dL.
As the blood sugar level in your body becomes critically low, you can experience symptoms like:
These symptoms result from mild-moderate hypoglycemia, which can be quickly treated by ingesting any sugary substance to bring the blood sugar to normal.
If left untreated, hypoglycemia can lead to more severe symptoms like:
Such symptoms will still require ingesting sugar to improve the blood sugar levels, but the patient must be hospitalized and monitored for a while.
Further negligence can even become fatal. The brain will be glucose-deprived for too long, and the body functions will begin to shut down.
Patients diagnosed with diabetes usually aren't oblivious to their condition. They're well informed about the early signs of hypoglycemia to quickly find a sugary beverage and seek medical advice if they get a glimpse of the symptoms.
However, the problem occurs during nighttime when the patient is sleeping. Most of the time, a diabetic patient will quickly wake up once their body starts sending all of those alarming signals.
Sometimes, the patient doesn't wake up, leading to a cascade of physical reactions that increase in severity until they pass away during sleep. This is known as dead-in-bed syndrome or DIB.
This harrowing expression describes the sudden deaths of young people with type 1 diabetes. In most cases, an insulin-dependent patient goes to bed with no signs of danger, only to be found dead the following morning.
DIB is quite rare and affects only 6% of insulin-dependent cases. However, this number isn't to be underestimated. There are 8.4 million people worldwide diagnosed with type 1 diabetes. Considering 6% of them would be at risk of DIB, this translates to 504,000 people.
Still, research was unable to provide a detailed explanation as to what the direct cause of DIB is. Yet, most cases had a history of type 1 diabetes.
This brings us back to the importance of continuous glucose monitors.
Most of these devices scan your blood glucose every five minutes, with some giving regular scans every minute or less. The latter devices are often prescribed to patients with a history of unexplained blood sugar fluctuations.
This continuous monitoring can be exceptionally important for those who might fail to identify the early signs of diabetes (like children and seniors).
Both age groups can be taught to seek help once the numbers on the device fall below or above a certain range, making managing the situation much easier.
The alarm-sending capability of these devices is the second line of defense. If the patient doesn't regularly check their screen for abnormal numbers, the device will alarm them when their blood sugar levels go out of range.
These alarms usually go to an external beeper or the patient's phone, but they can also be programmed to send alarms to other devices, like the phones of your family members or your doctor.
This is especially important if you're a heavy sleeper or your phone is switched off at night. It's also vital for children who may still need to own or hear their phones. The alarm would wake a parent or a sibling in the next room to help remedy a situation.
Understanding such patterns may help diabetic patients predict when their blood sugar levels are about to change.
For example, certain foods or physical or mental activities can trigger blood sugar fluctuations in some individuals. Without a continuous glucose monitor, identifying or even noticing those patterns is difficult.
This type of CGM has a short scan frequency. Most of them refresh the display on your screen every five minutes or so.
Most nighttime continuous glucose monitoring devices fall under this category.
These CGMs scan and display your blood glucose levels like real-time CGMs, but the intervals are longer (1-2 hours).
While those CGMs can still be worn during nighttime for patients with controlled diabetes, most are worn during the daytime as an extra assurance for the patient.
Diabetic patients wear these data-collecting CGMs to help their physician track the prognosis of their condition.
Some of them can still be programmed to send alarms should the blood sugar levels get out of range, but most are used primarily for treatment-monitoring purposes.
The majority of nighttime continuous glucose monitoring devices are in the real-time category. As such, all the information in this section primarily describes that type.
A CGM consists of three parts: the sensor, the transmitter, and the display device.
This is the part of the CGM that goes under the skin. It's usually in a hidden area where it won't be seen as much, typically the back of your arm or belly.
The sensor measures the fluid sugar inside your cells, typically similar to the blood sugar level.
Your physician will show you how to place the sensor under your skin the first few times.
Sensors have two types: disposable and implantable. The disposable ones are often cheaper, but they must be replaced every 7-14 days, depending on the manufacturer.
Implantable ones may last under your skin for up to half a year. They're convenient for the most part, but they're also quite expensive.
All the information gathered by the sensor is transmitted to an external device. This display could be a separate screen with the sensor in the box or your phone's screen through the manufacturer's downloadable application.
It's recommended to set up both and double-check readings.
The transmitter is the part responsible for transferring the information between the previous two parts. Some transmitters are permanently connected to the sensor, which will need to be replaced every time you change your sensor.
However, utilizing removable transmitters that you can use with multiple sensors is a more convenient option.
Nighttime CGMs can make all the difference because they watch over you when you're not watching over yourself.
Most are water-resistant, which adds to the convenience of keeping them in place while doing regular bathroom activities like washing your face or showering. However, going swimming while wearing CGMs will damage them since they're not completely waterproof.
However, CGMs still need to be supplemented by a regular glucometer test every once in a while. Remember, these devices measure the intracellular fluid glucose, which isn't always the same level despite being similar to the bloodstream glucose.
Please make sure that your CGM parts don't have any visible or detectable damage. The "detectable damage" is one that you can figure out when your readings don't make sense.
For example, registering low blood sugar levels after a large meal indicates something wrong with your CGM, rendering it unreliable.
CGMs save you a lot of headaches and time management by preventing you from manually checking your blood glucose with a glucometer.
Further, those with needle phobia will have their lives turned around by the reduced amount of needle pricks they get by using a CGM.
Also, pairing CGMs with a needle-free InsuJet or an insulin pump will make the life of a type 1 diabetic person much easier.
All that convenience comes with a cost, so it's important to set aside a budget for treating your diabetes. After all, no cost is too great to stay healthy and alive.
Despite the convenience, you'll still have to remove and insert the sensor, especially if you're using a disposable one.
Also, should any of the CGM parts go faulty, you'll have to replace those as well. This might take a bit out of the convenience of using CGMs, but they're still vital for those who suffer from unpredictable blood sugar fluctuations.
Not all bodies welcome having a foreign object stuck in the skin. Having a sensor will take time to get used to mentally and physically.
In the first few times, your skin might develop rashes, especially if you don't properly clean the area where you intend to place your sensor.
Also, on long-term usage, your skin might have a few wrinkles around the area where you constantly place your sensor. That's why having the sensor in a hidden or a less visible area is important.
Managing nocturnal blood sugar and nighttime continuous glucose monitoring devices go hand-in-hand, especially in cases where the patient has a history of abnormal blood sugar fluctuations.
Their benefits far outweigh their drawbacks, and they're constantly being developed to reduce any issues they might have.
If you're a diabetic patient or know someone who is, a nighttime CGM can be a great investment. And if you also want a needle-free option to take insulin, purchase an InsuJet kit today or reach out for more information.
Your cart is currently empty







