Revolutionizing Diabetes Management: The Power of Continuous Glucose Monitoring (2023)
|
|
Time to read 8 min
|
|
Time to read 8 min
Saying continuous diabetes management can mean the difference between life and death isn’t an exaggeration. With over 33 million people in Europe suffering from diabetes, 4.3 million in the UK alone, constantly monitoring blood sugar levels became necessary.
With needle-based glucometers being the most conventional method to monitor blood sugar for decades, those who don’t like needles tend to ignore that monitoring process just to avoid needle pain.
What’s the solution? A new device in diabetes technology is called a continuous glucose monitoring device. In this post, we’ll discuss how those CGMs revolutionize diabetes management.
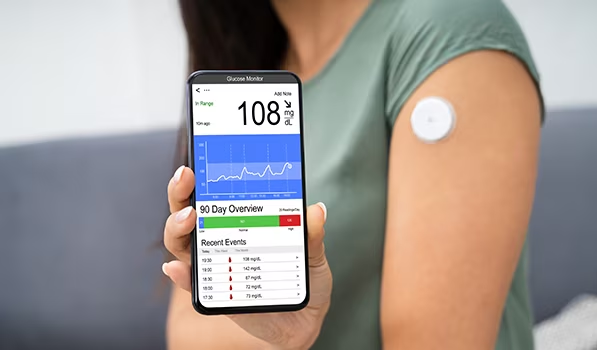
A CGM system is a device planted under the skin for continuous monitoring of your blood glucose throughout the day. The devices work by measuring the amount of glucose in the fluid between cells, which is often quite similar to the blood sugar levels in the bloodstream.
These devices would then periodically send the results to a glucose monitor, a smartphone, or an insulin pump.
The idea of using such devices is to make glucose monitoring more convenient. A diabetes mellitus patient is a lot more likely to keep their blood sugar levels in check if they can do so without the continuous finger pricking necessary for the standard glucose monitor to work.
It’s important to understand that a CGM and an insulin pump are different devices. A CGM will only monitor your blood sugar levels, while an insulin pump is an automated insulin delivery system.
CGMs have three primary parts that measure, transmit, and display blood sugar levels.
The first part is the sensor, which is inserted under the skin of your arm or belly. There are two types of CGM sensors: disposable and implantable sensors.
A disposable sensor uses a sticky patch like ours to cover wounds.
On the other hand, implantable sensors are often placed inside your body, which gives them the advantage of lasting more than a disposable sensor.
Regardless, both sensors must be replaced periodically, depending on the manufacturer.
The second integral part is the transmitter, which sends the information gathered by the sensor to the third part so it can be reviewed and monitored.
The transmitter is directly connected to the sensor, and they’re both placed under the skin. The information sent to the third display device is done wirelessly.
You’ll need to see the information gathered by your CGM, and that’s often done through a separate device. In most cases, this device is your smartphone through an application.
Some CGMs also send the information to a separate insulin pump to adjust the blood sugar levels when needed, which could be a lifesaver for type 1 diabetes patients.
While all CGMs measure your blood sugar levels, the means of how often they do so, how often they store the information, and how they display the information can differ.
These types of CGMs automatically measure blood glucose levels and send the information to the display device. The user doesn’t have to adjust, scan, or measure anything.
Intermittent scan CGMs also monitor blood sugar levels automatically. However, to get the results, the patient has to scan the CGM with a separate device, usually a receiver or a smartphone.
Data-collecting CGMs are useful tools to help your doctor monitor your condition. They work just like other CGMs, but the data gets sent to your doctor so they can monitor your condition.
Here’s why using a CGM is a good idea:
The most important advantage of continuous glucose monitoring is preventing diabetes complications. Diabetic complications arise when patients fail to monitor their blood sugar levels regularly, often from ignorance or needle phobia.
Diabetic patients who fear needles will be much less likely to monitor their blood glucose using conventional glucose meters. Those meters always require a needle prick, which is difficult for such people.
This makes them more susceptible to dangerous blood glucose fluctuations that could lead to high blood sugar (hyperglycemia) or dangerously low blood sugar levels (hypoglycemia).
However, when you use a needle-free glucose monitoring device (along with a needle-free insulin administration device), your diabetes will be a lot less impactful on your life.
Even with continuous monitoring, sudden blood glucose changes could still occur. CGMs reduce the risk of such dangerous fluctuations by sending alerts to the receiver screen.
This is especially useful if you have a child with type 1 diabetes and they get a sudden glucose drop overnight.
Once the blood sugar levels drop, the CGM will alert the parent in the other room to wake them up. These alerts often go through the silent phone modes, enhancing their safety.
It can also be useful for patients who don’t notice when their blood sugar levels suddenly change. If your doctor monitors your blood glucose readings through your CGM, they’ll warn you when your blood sugar gets to a dangerous level.
Some models even display how quickly your glucose levels are rising or dropping, which could help you predict when your blood sugar levels might fluctuate.
Using this feature, you can identify the activities/foods/situations that notably affect your blood sugar.
This can help you understand what to do, avoid, and how much insulin you’ll need after meals.
CGMs have come a long way in diabetes care since they were first invented, and it’s not a stretch to say that they have revolutionized diabetes management.
However, they’re not without their issues. Here are some things to keep in mind while using CGMs:
CGMs are fairly accurate, but they measure the glucose found in the body cells, which is often similar to the blood sugar levels, but not always.
Because of that, their accuracy is still somewhat inferior to the conventional blood sugar meters, which measure the sugar levels directly from the blood.
If you suspect your CGM is giving you inaccurate levels, a finger-stick test might be a good idea. Occasionally comparing your CGM and your glucometer results, even if you don’t suspect anything, can help you detect any abnormalities.
CGMs cost a fair amount more than your standard glucometer. Some models may be covered by your insurance, but you may have to pay a decent amount, especially if you rely on the disposable CGM.
If you’re using disposable CGM sensors, you must replace them periodically (typically every 7-14 days). This might inconvenience some people, which is why they might consider implantable sensors.
Still, despite lasting much longer than disposable sensors, implantable ones must be changed twice or thrice a year (some models can last up to 180 days).
Also, one of the three primary parts of the CGM might malfunction and require replacement. You or your doctor will notice when one of the parts is faulty when you consistently get inaccurate results.
Skin redness or irritation might occur if you’re using disposable CGMs. If that keeps happening, your doctor will prescribe you some medications to ease the process or recommend using implantable CGMs.
This section will provide the steps to use a continuous glucose monitor appropriately.
However, this will tackle the general idea, and it doesn’t replace your doctor’s advice, as models may have slight usage variations.
You place the sensor under the skin (usually hidden behind the arm) using an application designed for the process. Your doctor often does The first time; then, you’ll learn how to do it on your own with time.
After ensuring the sensor is in place, wear an adhesive patch to keep it fixed.
The device will take continuous readings (often every five minutes), and it’ll be your job to check these readings on your wirelessly connected display whenever possible. It’s best to do so after meals and any physical effort.
Based on the model, you’ll need to change the sensor every 7-14 days (not applicable for implanted sensors). Remember that some models' transmitters can be detached and used with new sensors.
Any patient who has diabetes can use CGMs to make their lives easier. However, in most cases, CGMs are prescribed by doctors to manage type 1 diabetes since it’s insulin-dependent.
With an insulin pump, CGMs can simplify the management of type 1 diabetes.
The pumps can be adjusted to administer emergency insulin doses if the CGM detects a sudden drop in blood sugar levels.
Also, CGMs can be used across all ages and down to two years old.
This depends on your condition. If you’re constantly having trouble monitoring your blood glucose or getting more blood sugar fluctuations than you like, CGMs might be a permanent solution for you.
Still, it’s not uncommon for doctors to prescribe CGMs for a specific data-collecting period to their patients. This is especially common in type 2 diabetes since it’s not insulin-dependent.
CGMs have some disadvantages, but safety isn’t one of them (except for the occasional skin rashes). As long as the skin surrounding the skin is clean, you should have no physical manifestations while using CGMs.
However, it’s up to you to periodically do a regular blood sugar test to check the accuracy of your CGM.
Most CGM systems are water-resistant but not waterproof. That means they can withstand regular water exposure from sweat, rain, and showers.
Just make sure not to submerge them underwater, as they’re not designed for this.
Continuous glucose monitoring shouldn’t be taken lightly. Letting go of your blood sugar can worsen your diabetic condition and even become life-threatening.
These CGMs have come a long way since they first appeared and are still constantly being improved. Pair them with insulin pumps or needle-free InsuJets to live as if you’re diabetes-free.
Your cart is currently empty






